Background:
Hypoglycemia is an easily identifiable and quickly reversible cause of seizures in the pediatric patient population. Current recommendations highlight the importance of identifying hypoglycemia prior to initiation of anticonvulsant therapy in children with suspicion for seizures. However, these recommendations conflict with prior research that suggest that very few pediatric patients with seizures require treatment for hypoglycemia. The investigators of this study hypothesized that hypoglycemia is an uncommon cause of seizures in the prehospital setting and they sought to derive an evidence-based algorithm for the evaluation of pediatric seizures by prehospital providers. Furthermore, the study creators hypothesized that repeat blood sugar testing in the ED was not indicated in patients who had return to baseline or normal mental status.
Methods:
This was a retrospective study, the investigators conducted a retrospective chart review for all consecutive pediatric patients (age 14 or less) with a prehospital complaint of seizure that presented to a busy county hospital and pediatric medical center in Los Angeles between January 2010 and January 2011. Information was collected regarding recorded age, sex, past medical history, GCS (mental status), prehospital glucose measurement, whether or not patient was seizing in the field, seizure duration, transport time, mental status on arrival, disposition and final diagnosis.
Key Results:
A total of 770 consecutive pediatric seizure patients were examined during the one year time period. The investigators presented the following important key findings:
· 521/770 (67%) of patients had a glucose recorded on chart review
· 84/770 (14%) were actively seizing on EMS arrival
· 4/770 (0.5%) of all patients were found to be hypoglycemic in the field (0.8% of patients with blood glucose reported)
· There was no statistically significant difference between blood glucose levels obtained in the field as compared to those in the ED
· Almost 80% of patients were discharged home from the ED
· The most common diagnoses were simple and complex febrile seizures
Takeways:
Among pediatric patients with a chief complaint of seizure, hypoglycemia was an extremely rare occurrence. Routine universal blood glucose testing for pediatric patients with concern for seizure prior to administering a benzodiazepine or who had returned to normal mental status was not supported based on the findings of this study. Furthermore, repeat blood glucose testing was not supported for patients who return to normal or baseline mental status.

What This Means for EMS:
Seizure is a common chief complaint encountered in the prehospital setting. While hypoglycemia has classically been taught to be an important cause of seizures, the results of this study suggest that hypoglycemia is not common in children who present with seizures or altered mental status. Furthermore, fingerstick blood glucose measurements can cause children to experience significant pain. The issue of universal fingerstick blood glucose measurements in patients who present with concern for seizure is also tied into false negative low glucose values which often require repeat testing in the emergency department contributing to increased length of stay. The investigators of this study postulate that routine blood glucose testing of all children in the prehospital setting who demonstrate normal or baseline mental status is not indicated. The detrimental effects of universal blood glucose testing extend beyond just pain and increased length of stay, but has also been linked to potentially delaying administration of antiepileptic medications in children with status epilepticus.
The investigators of the study formulated a new algorithm for prehospital management of the various classes of seizure patients: 1) patients actively seizing, 2) patients with GCS <15, 3) patients at baseline mental status.
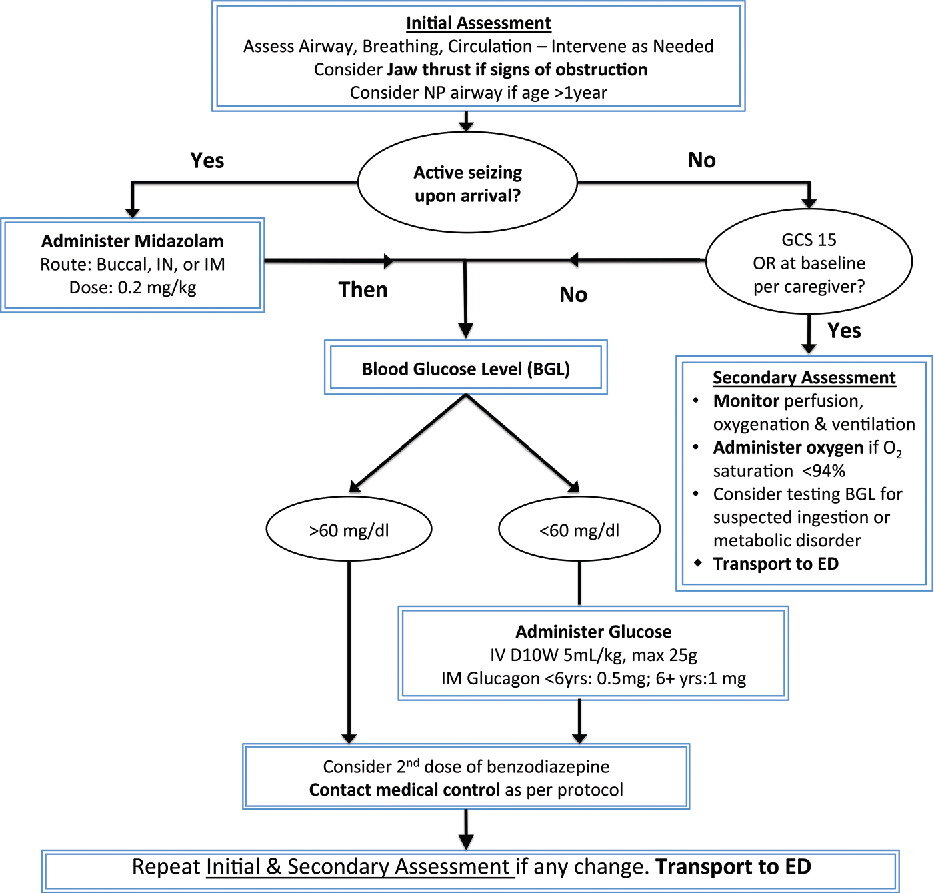
Figure 1 from Remick et. al.
Article Bites Summary by Al Lulla, MD (@al_lulla)


