David Wright, PA-C, NRP & Bridgette Svancarek, MD, FAEMS

“There should be a paramedic to Physician Assistant (PA) fast track!”
“PAs and paramedics do about the same job!”
“Isn’t a PA doing the same job as a paramedic, just in the hospital?”
“Paramedics are just as good as nurses”
“Why don’t we [paramedics] get paid like nurses””
Over time, I’ve heard it all. The questions, the comparisons, the ideas of a fast track curriculum to ultimately go from Paramedic to Physician Assistant (PA). It seems a natural progression. Back in 1965, the first class of PA’s was established by a physician at Duke University. [10] The class was composed completely of Navy Corpsman with substantial medical training. This is the same place we get military medical training from today. Years later there have been many EMS professionals that have left EMS to go to PA school. Personally, as a paramedic who went to PA school, I can offer some insight in to this line of thought. Today it is difficult for some of our paramedics to make the transition. While paramedics are trained to be effective Emergency Prehospital Medical Providers, they are often not required to take the advanced sciences, such as Organic Chemistry, Biochemistry, Physics, statistics and psychology, among others. For paramedics to be able to transition to a PA, there needs to be additional training provided, in addition to PA school.
Let’s take a dive into the idea of having EMS PAs, who Dr Mark Escott (Medical Director of Austin Travis County EMS) has appropriately named, Paramedic Practitioners.
Current EMS Education
Today, EMS education is primary classified as a technical career. Most paramedic programs are required to be accredited by the Commission on Accreditation of Allied Health Education Programs (CAAHEP). CAAHEP accreditation is recommended by The Committee on Accreditation for the EMS Professions (CoAEMSP). CoAEMSP currently does not require a college degree as part of their minimum standards for accreditation. In 2013, the National Registry of Emergency Medical Technicians (NREMT) transitioned to a national standard of 4 separate types of emergency medical provider [2,3,13,14] :
Emergency Medical Responder (EMR) – EMRs complete approximately a 48-60 hour course that trains them to provide immediate life saving care to critically ill patients. They are trained to treat the immediate threat while awaiting additional EMS resources. They can perform basic interventions with minimal equipment.
Emergency Medical Technician (EMT) – EMTs complete approximately a 150-190 hour course that trains them to provide out of hospital emergency care and transport of the critical patients. They have basic skills and knowledge designed to stabilize and transport patients in both the emergency and non-emergent setting. They can perform interventions with basic equipment on an ambulance.
Advanced Emergency Medical Technician (AEMT) – AEMTs complete approximately 150-250 hour course that trains them to provide basic and limited advanced emergency care and transportation skills for the critical patients. They have additional training in comparison to EMTs and can perform basic and advanced interventions with both basic and advanced equipment normally on an ambulance.
Paramedic – Paramedics complete approximately a 1000 hour course that trains the allied health professional to provide advanced emergency care for critical patients. They have complex knowledge and skills to provide quality patient care and safe transport. They can perform both basic and advanced interventions and can utilize basic and advanced equipment found on an ambulance.
Specialty Paramedics are a relatively newer concept. They further specialize in specific types of care. In some states, there are certification courses and examinations that exist for specialties such as tactical medicine, community paramedicine, and critical care paramedicine. [3] There are no defined national standards regarding these specialty paramedics. While there may be a certification exam that is available, it may not be required to be obtained prior to practicing in that field. Without national standards, there is a lot of variation in the teaching and education of these types of providers. Some are short courses that could be offered in a weekend, while others are months or longer in duration.
Current PA Education
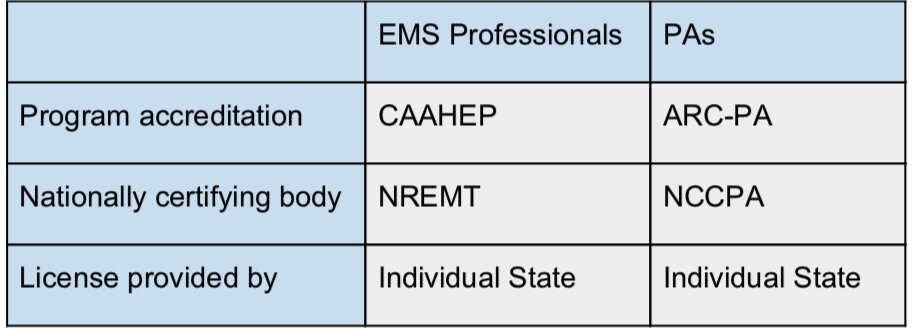
Table 1: Accreditation, Certification and Licensing Bodies for Paramedics and Physician Assistants.
Physician Assistant Education, on the other hand, is accredited by the Accreditation Review Commission on Education for the Physician Assistant (ARC-PA) and is typically a masters of science degree, with program length averaging 24-36 months. Currently most PA programs focus on general medical knowledge, such that pertains to primary care. [6] During the clinical portion of the program, multiple clinical rotations are complete in various specialties. These specialties include Emergency Medicine, Pediatrics, Obstetrics/Gynecology, Family Medicine, and Surgery. Many programs also allow for the student to have input in their clinical time and have a “student directed” clinical rotation, where the student can revisit a previously completed specialty, or experience something they have a personal interest in.
Once the professional program is completed, students are eligible to sit for the Physician Assistant National Certifying Exam (PANCE) exam. This exam is provided by the National Commission on Certification of Physician Assistants (NCCPA) who acts as the certifying body for PAs. NCCPA is to PAs what NREMT is for EMS professionals [Table 1].
Comparison to Nursing
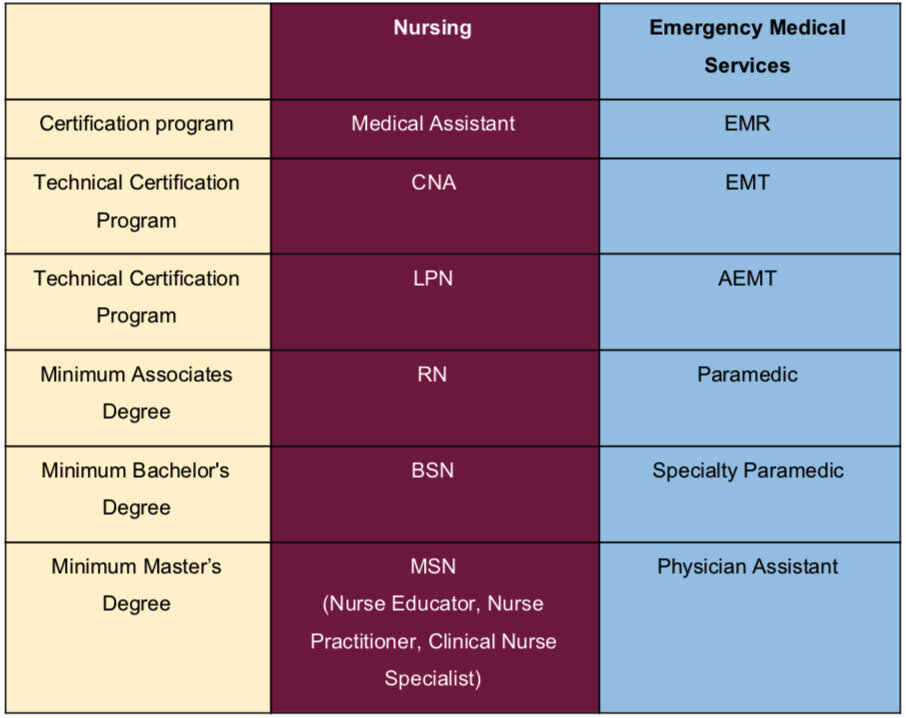
Table 2: Proposed comparison of nursing education to EMS education. Currently, in most states, paramedic is not currently an associates degree and there is no bachelor’s degree requirement.
Often our EMS profession is compared to the age old profession of nursing. While the concept of nursing has been around for a long time. The American Nurses Association was created in 1896, compared to the creation of EMS in 1966. [7,11] Today nursing has a hierarchy that can be compared to that in EMS, but EMS seems to comparatively fall short in education requirements. Nursing has placed value on formalized post secondary education. Nursing organization starts at Certified Nursing Assistant (CNA) and continues to Licensed Practical Nurse (LPN), Registered Nurse (RN), Bachelor of Science Nursing (BSN), Masters of Science:Nursing (MSN). This organization is very similar to EMS from EMR, EMT, AEMT, Paramedic and the proposed Paramedic Practitioner.
A proposed example comparing the Nursing education to EMS education is outlined in Table 2.
Proposed Educational Requirements
In 2018, the National Association of EMS Educators (NAEMSE), the National EMS Management Association (NAEMSE), and the International Association of Flight and Critical Care Paramedics (IAFCCP) released a joint position paper supporting the advancement of paramedics from a technician level program to a degree profession. [9] In 2013 NREMT changed the title of the Paramedic from EMT-P to Paramedic, in an effort to enhance the title by removing the technician label. [13]. In 2010, CoAEMSP recommended that all accredited paramedic programs be offered college credit of 30 credit hours. [12] This eases the transition from a technical program to degreed profession. Today there are many colleges/universities that currently offer Associate\’s Level degrees (usually Associate in Applied Science or Associate of Science) in Paramedic Care. According to the National Association of EMTs (NAEMT), there are currently only about 25 EMS four year degree programs or higher. [8]
Below is a proposed degree pathway for each of the level of EMS providers allowing smooth transition from paramedic to PA:
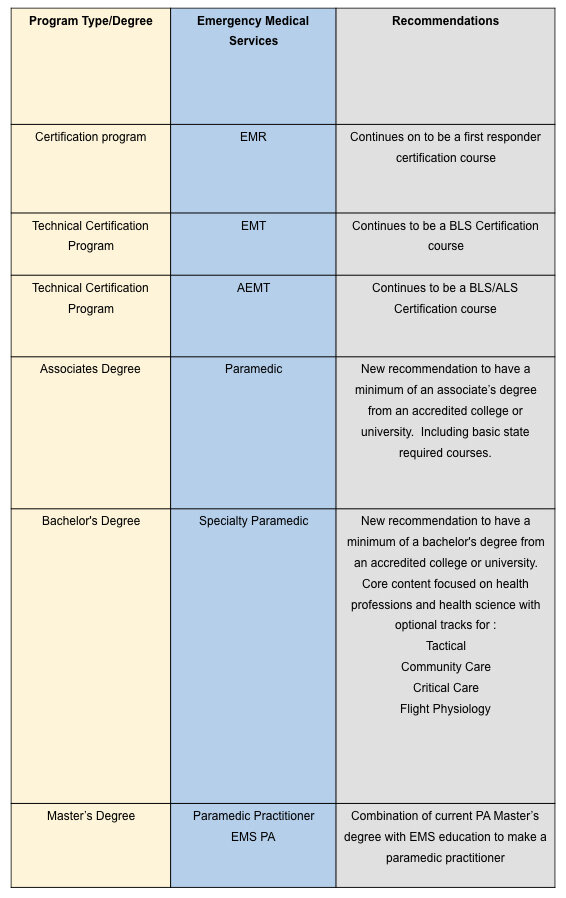
Table 3: Proposal for future EMS Degree Pathway
Logistical Considerations for Requiring EMS Degrees
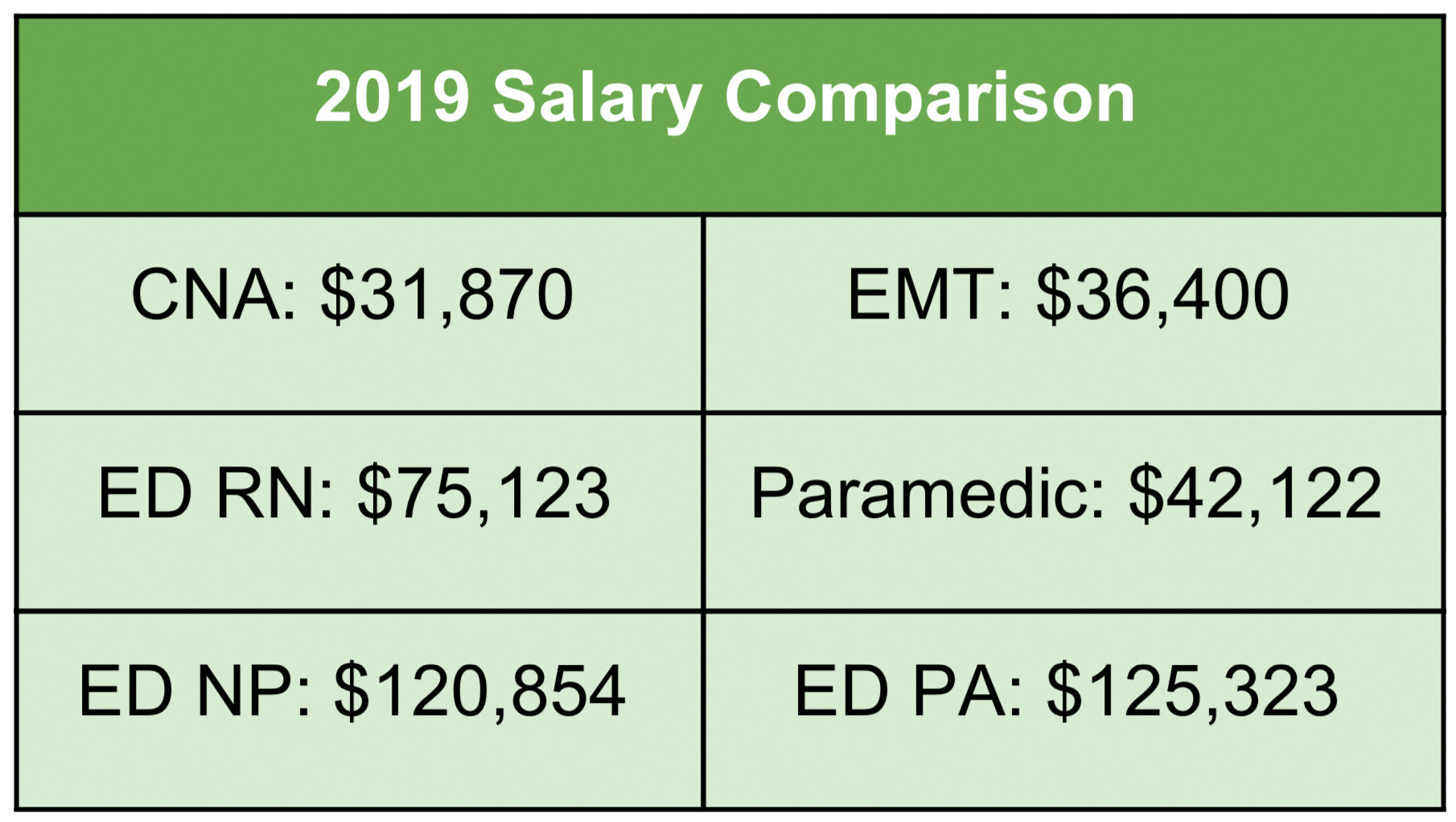
Table 4: 2019 Salary Comparison between Nursing and EMS providers (All data sourced from Salary.com, average annual yearly salary)
Of the largest hurdles to requiring degrees for EMS education, time and money are at the forefront. NAEMSE has published a position paper stating on-line/distance education is one potential solution. [15] With the immersion of technology in the educational world, online programs are becoming more popular, and there are less challenges faced when moving these “additional courses” online. This would allow for them to be completed in a flexible, asynchronous manner, to anyone with a computer. This style of learning, would be able to accommodate the abnormal scheduling of many EMS providers.
Money is another limiting factor for EMS degrees. Many opportunities for assistance with finances for degrees are available, especially for those who currently do not hold a degree. Examples of such funding include Federal PELL grants, workplace assistant, community based scholarships, school based scholarships. Each one of these requires a small amount of work on behalf of the student, but there are many available opportunities for those willing to look for them.
When the salaries between nursing and EMS providers are compared [Table 4], it appears that in the technical programs (CNA vs EMT), our EMS providers are making 14% more than CNAs. An even smaller pay gap was identified with the Master’s Level providers (ED Nurse Practitioners vs the ED Physician Assistants) at 3%. Meanwhile the Associate’s Degree ED nurses compared to the technical program Paramedic had a significant pay gap with a 78% pay difference in the nursing favor.
Can an EMS Practitioner be a reality?
In short, YES! It is possible that today, an EMS Paramedic Practitioner be a reality, in fact, there are some systems utilizing PAs in EMS at this time. Yet, there are still some challenges before a well defined pathway may become available nationwide. Currently, many of these Paramedic Practitioners are former Paramedics who continued on with their schooling to become a Physician Assistant. A master’s degree PA with a Bachelor\’s degree in EMS can easily be the paramedic practitioner of the future. Another option is to customize a current PA program into having more of an EMS focus. Instead of having the aforementioned “student directed” clinical experience, this is then substituted for an EMS rotation. In place of the multiple rotations in family medicine, there would be greater emphasis on emergency and unplanned medicine.
Having this defined pathway may lead to viable, life long careers with advancement options for EMS providers. This could help combat the long standing feeling of the EMS profession having limited career progression.
It is likely to see more of these ideas emerging. With the implementation of programs like Emergency, Triage, Treat and Transport (ET3) model and alternative transport destination protocols, along with an increase in ED volumes, and increased wait times speciality care paramedics and paramedic practitioners are going to be playing a more critical role. As these programs grow and mature, there will be an increased need for these levels of EMS providers. Implementation of the above proposal can ease their transition into these roles.
There is no better time than now to reflect and decide in what direction we want our profession to head.

References
-
Committee on Accreditation for the EMS Professions (2019) CAAHEP Standards & Guidelines. Accessed from: https://coaemsp.org/caahep-standards-and-guidelines#1
-
National Highway Traffic Safety Administration (2007) National EMS Care Content. Accessed from: https://www.ems.gov/pdf/education/EMS-Education-for-the-Future-A-Systems-Approach/ National_EMS_Core_Content.pdf
-
International Board of Specialty Certification (2020) Tactical Paramedics. Accessed from: https://www.ibscertifications.org/roles/tactical-paramedic
-
International Board of Specialty Certification (2020) Community Paramedics. Accessed from: https://www.ibscertifications.org/roles/community-paramedic
-
International Board of Specialty Certification (2020) Critical Care Paramedics. Accessed from: https://www.ibscertifications.org/roles/critical-care-paramedic
-
Physician Assistant Education Association (2013) Physician Assistant Educational Programs in the UInited States. Accessed from: https://paeaonline.org/wp-content/uploads/2016/10/27th-Annual-Report.pdf
-
American Nurses Association (2020) The History of the American Nurses Association. Accessed from: https://www.nursingworld.org/ana/about-ana/history/
-
National Association of Emergency Medical Technicians (2019) Degrees in EMS. Accessed from: https://www.naemt.org/about-ems/degrees-in-ems
-
Sean M. Caffrey, Leaugeay C. Barnes & David J. Olvera (2018): Joint Position Statement on Degree Requirements for Paramedics, Prehospital Emergency Care, DOI: 10.1080/10903127.2018.1519006
-
American Academy of Physician Assistants (2020). History of the PA Profession. Accessed from: https://www.aapa.org/about/history/
-
National Highway Traffic Safety Administration (1966) Accidental Death and Disability: The Neglected Disease of Modern Medicine. Accessed from: https://www.ems.gov/pdf/1997-Reproduction-AccidentalDeathDissability.pdf
-
Committee on Accreditation for the EMS Professions (2010) Articulation Agreements: The Path to Offering College Credit for Your Accredited Paramedic Program. Accessed from: https://coaemsp.org/?mdocs-file=1368
-
National Registry of Emergency Medical Technicians (2013) Transition Policy. Accessed from: https://www.nremt.org/rwd/public/document/policy-transition
-
National Highway Traffic Safety Administration (2007) National EMS Scope of Practice Model. Accessed from: https://www.nhtsa.gov/people/injury/ems/EMSScope.pdf
-
National Association of EMS Educators, Position Paper on the Use of Internet Based Distance Learning in EMS Education., Pittsburgh, PA, 2003. Accessed from: https://cdn.ymaws.com/naemse.org/resource/resmgr/Docs/DLPositionPaper111003.pdf


