
by Maia Dorsett, MD PhD (@maiadorsett)
Recap of the Case:
A 64 yo male is having dinner with his family when he begins to feel lightheaded and nauseated. As he stands up to leave the table, he collapses to the ground. His family calls 911. As he is unresponsive with agonal respirations, the call is dispatched as a cardiac arrest and the patient\’s family is instructed to perform CPR via pre-arrival instructions.
On EMS arrival, the patient is found to be pulseless. Compressions are continued while the patient is connected to the monitor. The EMS supervisor arrives on scene shortly after with a newly purchased mechanical CPR device.
Should the mechanical CPR device be used? If so, when should it be applied?
Do you have a protocol dedicated to use of mechanical CPR? If you utilize mechanical CPR, how do you integrate it into your cardiac arrest resuscitation so as to minimize interruption of chest compressions?
Review:
High quality compressions of adequate depth, rate, recoil and with minimal interruption are crucial to neurologically-intact survival from out of hospital cardiac arrest (OHCA). Quality compressions require considerable physical effort on the part of providers leading to decreased compression quality over time. A number of mechanical CPR devices have been developed with the goal of maintaining compression consistency and off-loading the work of compressions [1]. However, when applied to all patients with cardiac arrest, mechanical CPR is equivalent or inferior to manual CPR in achieving neurologically-intact survival.
The first large trial to examine the effect of mechanical CPR on cardiac arrest outcomes was a multicenter randomized control trial in the United States and Canada [2]. The trial enrolled patients from 2004 to 2005. Individual stations within each site were randomized to manual CPR or mechanical CPR with an AutoPulse band device, with subsequent alternation between intervention and control groups. They found no difference in the primary outcome of 4 hr survival between manual and mechanical CPR (N=1071; 29.5% vs 28.5%; P=.74), but found that an overall lower rate of neurologically-intact survival among those patients who received mechanical CPR (3.1 % for mechanical CPR vs. 7.5% for manual CPR , p=.006). The study was terminated early because of poorer neurologic outcomes in the mechanical CPR group.
Following this, three randomized control trials (CIRC, LINC and PARAMEDIC) found that mechanical CPR was non-inferior to manual CPR.
The CIRC trial was a randomized control trial of mechanical CPR using the Autopulse band device versus standard CPR [3]. It included all 4231 patients with arrests of presumed cardiac origin. Patients were randomized by sealed envelopes opened after manual compressions were initiated. They found no difference in survival to hospital discharge between mechanical and manual CPR (OR for mechanical compared with manual: 1.06, 95% CI 0.83-1.37). For the secondary outcome of good neurologic outcome (defined as a modified Rankin score of < 3 at discharge from the hospital), there was no difference between mechanical and manual CPR (OR for mechanical compared with manual; aOR 0.80, 95% CI 0.47–1.37).
Unlike the CIRC trial, the LINC trial (Lucas IN Cardiac arrest) used the plunger-type Lucas device. 2593 patients were randomized using a sealed envelope after initiation of manual compressions [4]. The mechanical compression arm of the study varied more than just the mode of CPR. In the Lucas arm, the first defibrillation shock was delivered during ongoing compressions without pausing to check the heart rhythm and CPR cycles were extended to 3 minutes between subsequent rhythm checks. When comparing the two arms, the authors found no difference between 4 hr survival (307/1300 [23.6%] vs 305/1289 [23.7%]; risk difference, −0.05%; 95% CI, –3.3% to 3.2%; P<.99) and neurologic outcome at hospital discharge (108/1300(8.3 %) vs. 100/1289 (7.8%), risk difference, 0.55; 95% CI−1.5% to 2.6%; p = 0.61). Mechanical and manual CPR groups were similar in the proportion of patients with witnessed arrest, bystander CPR and shockable rhythm.
The PARAMEDIC trial also compared mechanical CPR with a LUCAS device to manual compressions [5]. Randomization was done with a computer-generated randomization sequence that assigned particular vehicles to carry the device. The study enrolled 4471 patients with similar baseline characteristics. Manual compressions were initiated until the device could be placed. During pauses, if a shockable rhythm was found, the LUCAS was turned back on and defibrillation took place with ongoing mechanical CPR. The study found no significant difference in the primary outcome of survival to 30 days (aOR 0.86, 95% CI 0.64-1.15). Survival with favorable neurologic outcome at 3 months was lower in the group receiving mechanical CPR (aOR 0.72, 95% CI 0.52-0.99).
Two subsequent meta-analyses found no difference between manual and mechanical CPR on favorable neurologic outcome [6,7].
In an effort to compare outcomes for patients receiving manual versus mechanical CPR in the “real world” outside of the well-trained and monitored randomized control trials, two recently published studies retrospectively evaluated outcomes from patients in the CARES registry.
First, an observational cohort study of all cardiac arrests treated in the state of Utah from May 2012 through June 2015 tracked via the CARES registry was published in January 2016 [8]. This included adult patients with non-traumatic arrest who were either defibrillated with an AED or received chest compressions from a prehospital provider. They analyzed 2600 resuscitation attempts. Overall, mechanical CPR (predominantly with the AutoPulse device) was used in only 16% of all arrests. Patients who received mechanical CPR also were more likely to have several poor prognostic factors; their arrests were less likely to be witnessed, more likely to present with asystole and require more interventions (ACLS medications, advanced airway placement). The authors therefore used a regression model with weighted propensity to scores in order to control for possible confounders/selection bias – witnessed arrest, bystander CPR, deliver of bystander AED shock, initial shockable rhythm. Using this approach, the authors found that the adjusted relative risk for neurologically-intact survival with mechanical CPR compared to manual CPR was 0.41 (95% CI, 0.24 – 0.70, p=0.001). In a subgroup analysis, mechanical CPR was still associated decreased likelihood of neurologically-intact survival in patients with a shockable rhythm on initial check (aRR 0.47, 95% CI 0.25 – 0.86, p=0.001) and EMS-witnessed arrests (RR 0.18, 95% CI 0.08-0.40), p< 0.0001).
More recently, the analysis of the CARES registry and been expanded to a national scale [9]. A retrospective study of CARES registry data from January 2013 to December 2015 included an evaluation of outcomes in 80,861 patients. Using a multivariable regression model to control for arrest characteristics – age, arrest location, bystander CPR, AED use, initial rhythm, witnessed arrest, post-arrest targeted temperature management, successful placement of an advanced airway – they found that patients who received mechanical CPR were less likely to survive to hospital discharge (7.0% vs. 11.3%, p < 0.001) or have neurologically-intact survival (5.6% vs. 9.5%, P < 0.0001).
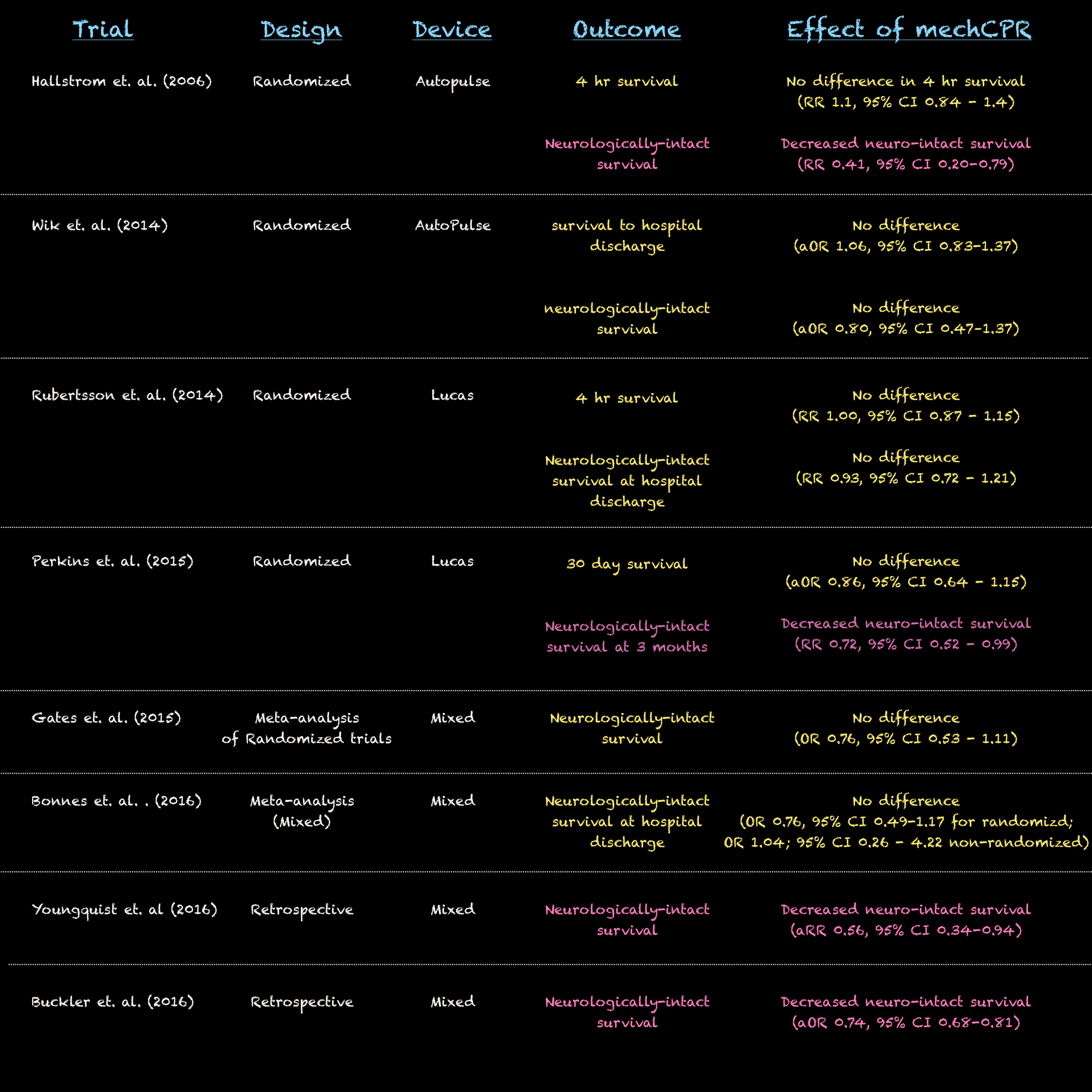
The above studies not only find lack of benefit, but also potential harm in the employment of mechanical CPR devices. Should this be the end of their use? Not necessarily, but these studies should make us strongly consider why use of mechanical CPR may be associated with worse neurologic outcomes.
Comments in response to the discussion forum questions focused on 3 key issues surrounding employment of mechanical CPR: Training, Personnel and potential need for transport.
Training and Personnel:
“The first thing I would like to know is do all of the crew members have training and knowledge of the device to be used? Does this device come on a fly car such as a physician vehicle or is this something that all units and crew members have practiced beforehand and is available to every transporting unit? Was the device implemented yesterday or 6 months ago? To maximize easy of use and decrease interruption of chest compressions, a comprehensive crowd knowledge and familiarity would be best. “
“Locally, in accordance with our statewide protocols, we limit use of mechanical compression devices during the first 10 minutes of resuscitation (link). With more time into an arrest, this generally also means more time for hands to arrive to assist. Having more crew members to assist, the better. In using the LUCAS device, we have found that having at least four people is ideal.” – J. Escajeda
The association of mechanical CPR with worse neurologic outcome may be due to prolonged interruption of compressions when the device is applied. Indeed, the one site with a quality improvement initiative to minimized interruption in compressions in the Hallstrom et. al. trial changed their protocols mid-study as they found that there was a prolonged time without compressions while deploying the mechanical CPR device [2]. This does not mean that sufficient training cannot improve the efficiency and coordination with which the device is placed – but this requires recognition that funding for a mechanical CPR device must be accompanied by funding to provide adequate training in its use and ongoing quality review of effect on local outcomes.
Potential Need for Transport:
“The other question that comes to mind is what are your end-points to this particular arrest? Is this an organized rhythm (along with the mentioned witnessed arrest, bystander CPR). We know that there is no demonstrated benefit to a device [Perkins, Rubertsson], however, a role could be to maximize compressions during transport, a time when maintaining compression quality is difficult. Is this someone that is being transported to the hospital for other interventions such as ECPR?” – J. Escajeda
While staying on scene until ROSC or termination of arrest may be appropriate for the most cardiac arrest cases, there is emerging evidence that some patients with refractory arrest should be considered candidates for advanced therapies including ECMO, percutaneous coronary intervention or pulmonary embolectomy. Recently, initial results of the CHEER trial (mechanical CPR, Hypothermia, ECMO and Early Reperfusion) therapy carried in out Australia were published [10]. This pilot trial of a very select group of patients (age 18-65 years, cardiac arrest due to suspected cardiac etiology, chest compressions within 10 minutes, initial rhythm of ventricular fibrillation, absence of pre-existing non-cardiac morbidities affecting activities of daily living, and general gestalt by a critical care physician that the etiology of cardiac arrest would be reversible if veno-arterial ECMO and definitive treatment could be provided immediately) included 11 patients with OHCA. There were 5 survivors, all of whom were discharged directly home with full neurologic recovery, despite a median collapse to hospital arrival of 48 minutes (IQR 23-64).
As transport is a particularly difficult time to maintain quality compressions, mechanical CPR may be of benefit in the group of patients who are being transported (including post-ROSC patients who are high risk of re-arrest en route to the hospital).
Take Home: In general, mechanical CPR has no proven benefit in cardiac arrest and is associated with lower neurologically-intact survival in some studies. Mechanical CPR may best be utilized in the care of patients requiring transport, and EMS protocols should stress application of the device in a manner that leads to minimal interruption of compressions. For an example protocol, see (this protocol) from Sedgwick County EMS (written by Sabina Braithwaite, modified from Michael Levy’s Anchorage protocol).

Other #FOAMed posts on Mechanical CPR
EM Nerd: The Case of the Bridge to Nowhere
REBEL EM: The Death of Mechanical CPR?
References:
1. Ward, K. R., Menegazzi, J. J., Zelenak, R. R., Sullivan, R. J., & McSwain, N. E. (1993). A comparison of chest compressions between mechanical and manual CPR by monitoring end-tidal PCO2 during human cardiac arrest. Annals of emergency medicine, 22(4), 669-674.
2. Hallstrom, A., Rea, T. D., Sayre, M. R., Christenson, J., Anton, A. R., Mosesso, V. N., … & Yahn, S. (2006). Manual chest compression vs use of an automated chest compression device during resuscitation following out-of-hospital cardiac arrest: a randomized trial. Jama, 295(22), 2620-2628.
3. Wik, L., Olsen, J. A., Persse, D., Sterz, F., Lozano, M., Brouwer, M. A., … & Travis, D. T. (2014). Manual vs. integrated automatic load-distributing band CPR with equal survival after out of hospital cardiac arrest. The randomized CIRC trial. Resuscitation, 85(6), 741-748.
4. Rubertsson, S., Lindgren, E., Smekal, D., Östlund, O., Silfverstolpe, J., Lichtveld, R. A., … & Halliwell, D. (2014). Mechanical chest compressions and simultaneous defibrillation vs conventional cardiopulmonary resuscitation in out-of-hospital cardiac arrest: the LINC randomized trial. Jama, 311(1), 53-61.
5. Perkins, G. D., Lall, R., Quinn, T., Deakin, C. D., Cooke, M. W., Horton, J., … & Smyth, M. (2015). Mechanical versus manual chest compression for out-of-hospital cardiac arrest (PARAMEDIC): a pragmatic, cluster randomised controlled trial. The Lancet, 385(9972), 947-955.
6. Bonnes, J. L., Brouwer, M. A., Navarese, E. P., Verhaert, D. V., Verheugt, F. W., Smeets, J. L., & de Boer, M. J. (2016). Manual cardiopulmonary resuscitation versus CPR including a mechanical chest compression device in out-of-hospital cardiac arrest: a comprehensive meta-analysis from randomized and observational studies. Annals of emergency medicine, 67(3), 349-360.
7. Gates, S., Quinn, T., Deakin, C. D., Blair, L., Couper, K., & Perkins, G. D. (2015). Mechanical chest compression for out of hospital cardiac arrest: systematic review and meta-analysis. Resuscitation, 94, 91-97.
8. Youngquist, S. T., Ockerse, P., Hartsell, S., Stratford, C., & Taillac, P. (2016). Mechanical chest compression devices are associated with poor neurological survival in a statewide registry: A propensity score analysis. Resuscitation, 106, 102-107.
9. Buckler, D. G., Burke, R. V., Naim, M. Y., MacPherson, A., Bradley, R. N., Abella, B. S., & Rossano, J. W. (2016). Association of Mechanical Cardiopulmonary Resuscitation Device Use With Cardiac Arrest Outcomes. Circulation, 134(25), 2131-2133.
10. Stub, D., Bernard, S., Pellegrino, V., Smith, K., Walker, T., Sheldrake, J., … & Cameron, P. (2015). Refractory cardiac arrest treated with mechanical CPR, hypothermia, ECMO and early reperfusion (the CHEER trial). Resuscitation, 86, 88-94.


